Every 20 seconds in the world, there’s a lower-limb amputation due to diabetes. As one of the most severe chronic diseases in the world, diabetes affects the entire human body and is one of the conditions that would benefit the most from connected care solutions.
Connected care is a suite of digital products that support the collecting, monitoring and analyzing of health data at the point of care. Examples include glucose monitors, various patient apps, sensor technology, and activity trackers.
We got together with Chris Henderson, Global Digital Health Innovation Leader at Smith & Nephew and Digital Health Advisor at GrowthRide, to offer insights on how connected solutions can shape the future of medical care. We talked to Chris about how digital solutions may reach their full potential in the clinical realm. We believe that with an empathic understanding of how diabetes is managed, including the breadth of challenges patients face on a daily basis, we could shine a light on the potential of connected solutions as the future of chronic illnesses care.
How far can diabetes reach?
From head to toes
A global challenge
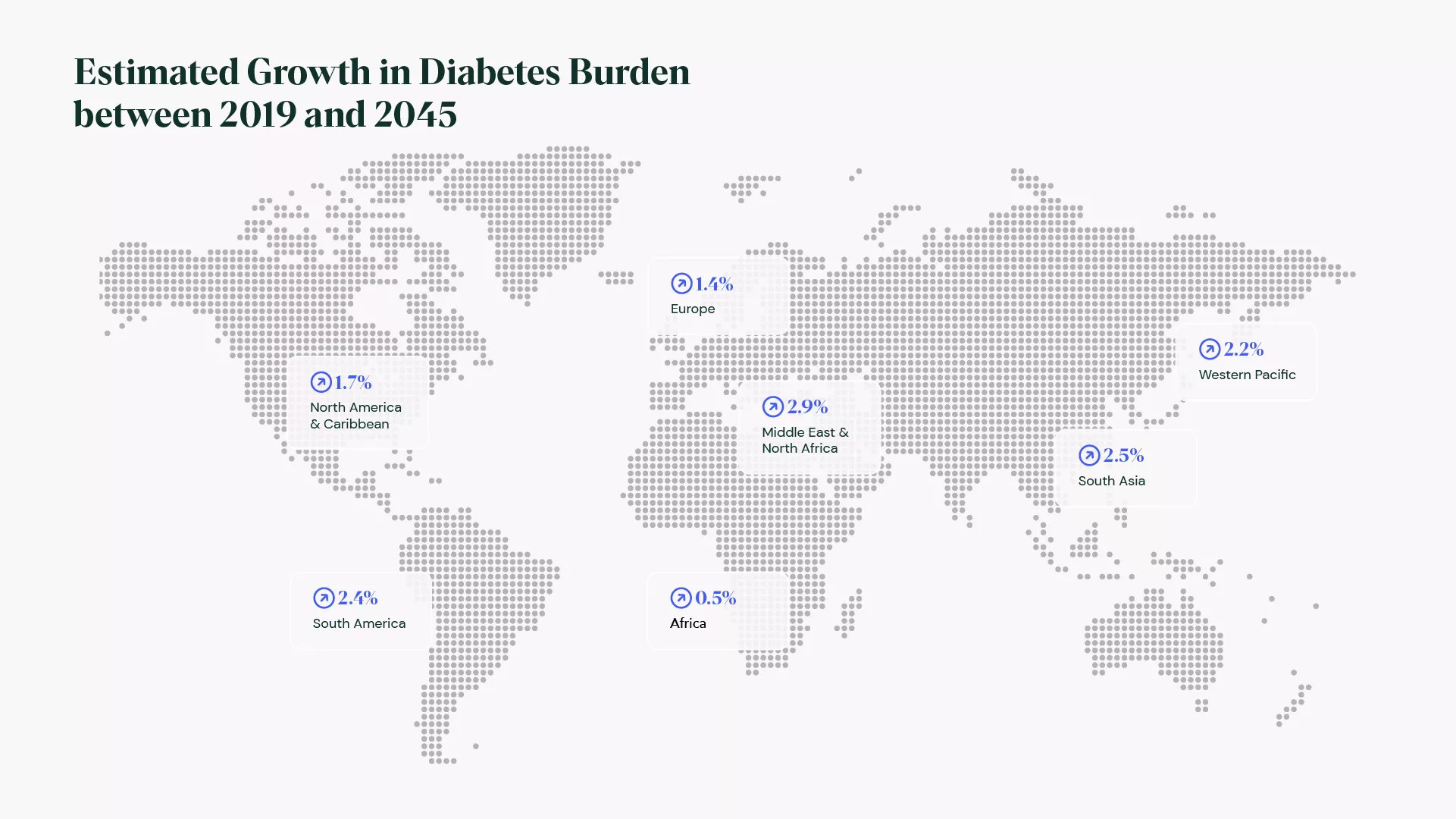
The severity of diabetes isn’t the only element that makes this a challenging condition. In the past few years, the increasing rate of diabetes diagnoses has been alarming, and the steepest curve is found in countries where healthcare systems are most vulnerable.
Additionally, the pandemic decreased the number of in-person healthcare visits, resulting in missed or delayed diagnoses and treatment opportunities. Creating new ways to address this global patient care is imperative.
With a large gap between known diabetes patients and actual cases, and the number of people affected on the rise, healthcare institutions and governments will be forced to respond to bigger healthcare demands in new innovative ways.
The lack of modern diabetes care solutions is a challenge for all stakeholders, affecting patients in all areas of their lives, and impacting the economical structure of healthcare ecosystems around the world.
Adapted from World Economic Forum
Connected care could be the answer
When it comes to diabetes management, face-to-face consultations remain the largest interactions, while community engagement, caregiver support, and patient-driven care remain relatively underutilized.
This is where connected care comes in as an opportunity to alleviate the burden on the medical system, and facilitate lifestyle habits for post-diagnosis diabetic care. Connected care also drives health equity, with solutions enabling broader access to care for deprived patient populations.
Designing a successful connected solution would radically shift the engagement between patients and health systems, impacting all medical specialties involved in treating this chronic disease. In the end, the success of connected solutions will be measured by their ability to integrate chronic disease management and personalized care.
What the future of connected healthcare could look like
In the last couple of years, we saw a dramatic acceleration in the adoption of digital solutions in the medical space. Driven by behavioral health, the success of connected care is measured according to how seamlessly they can fit into patients’ daily routines. Connected solutions are already offering significant changes to the healthcare landscape, such as digital patient records, or clinical appointments management, but when it comes to making a significant impact on the patient journey, there’s still a long road ahead.
The five pillars of connected care
Because diabetes care is the most complex environment for connected solutions, solving this challenge represents a cornerstone to build the future of connected care overall. What we call the pillars of connected care will be guidelines used as a driving force, so digital solutions can be designed not only for diabetes patients, but for any kind of chronic ailment.
From virtual coaching, to the logistics of how patients get their supplies, you could argue that connected solutions would break the in-person relationship between patients and practitioners. We argue that it could even make it stronger. Ask yourself, do diabetes patients really need a doctor’s appointment to get dieting tips? Having a solution that takes care of these kinds of processes doesn’t need real-time involvement from practitioners, reducing patients’ time spent on consultations, and freeing up doctors’ time for more pressing issues.
The meaning of comprehensive connection
We’ve mentioned how digital measures have been taking up more and more space when it comes to medical innovation. However, as a multi-specialty disease, diabetes care is still a major challenge. Diabetics are prone to head-to-toe problems, but asking them to manage a unique digital platform for each concern while making the time to drop their kids at school and go to work is beyond unrealistic.
These patients’ lives could be changed if the future of connected care is comprehensive and unified. It’s a matter of how well-connected digital solutions will be, integrating all of their needs into a single place. This isn’t just a theory that would impact the workflow in hospitals and clinics, it could change the lives of over 500 million people across the world.
A less spoken about, but equally important, element of connected solutions is the sense of community support. These spaces create a safe haven, a place for patients to connect with people undergoing similar struggles and concerns.
And, because connected solutions are data-driven, these spaces would not only bring support to patients, but generate enough information so that future solutions answer people’s medical, but also emotional, needs.
New solutions bring on new challenges
Breaking the traditional challenges in medical care means designing solutions for hybrid spaces. These should be environments that integrate patients, doctors, hospitals, insurances, providers, and more – where all are connected to all.
The future of diabetes care is being shaped today
Moving forward in a digital world means shaping connected solutions that redefine the future of healthcare. Everyone has a role to play: companies must build bridges across the health ecosystem to usher in the connected care era. At Board of Innovation, we solve problems through human-centric solutions. Connected solutions might be our way to imagine a new way for chronic disease management, addressing life challenges where life happens.